 |
Cardiac
troponins (cTn) are specific for myocardial damage.1 cTn measurements
have prognostic value2 and indicate the response to a range of treatment
modalities including low-molecular-weight heparins,3 glycoprotein IIb/IIIa
antagonists4,5 and revascularization.2,6,7 How should cTn measurement
be incorporated into routine clinical practice, and what is the likely
impact on the laboratory?
cTns
appear to be the “wonder test.” As they become more widely used, confusion
has arisen in the minds of some cardiologists and general physicians who
equate the presence of an elevated cTn with the diagnosis of acute myocardial
infarction, and the absence of cTn with no ischemic heart disease. Unfortunately,
this quest for diagnostic certainty is doomed to failure, as AMI remains
a clinical diagnosis. This fact is recognized in the recent document of
the joint committee of the European Society of Cardiology and American
College of Cardiology redefining AMI.8 The elevation of cTns
also occurs in a range of conditions other than acute coronary syndrome
(ACS), varying from the glaringly obvious, such as myocardial trauma (whether
from a knife through the heart or the machinations of a cardiothoracic
surgeon), through cocaine overdose (causing intense coronary vasoconstriction)
to myocarditis.
This ambiguity is easily resolved by dividing the causes of cTn elevation
into three categories. In primary ischemic cardiac injury (PICI), cTn
elevation occurs as a result of a ruptured coronary plaque. Secondary
ischemic cardiac injury (SICI) is cardiac injury arising as a result of
ischemia not primarily due to a ruptured plaque. Finally, nonischemic
cardiac injury (NICI) is injury caused by direct cardiac damage. Examples
appear in Table 1.
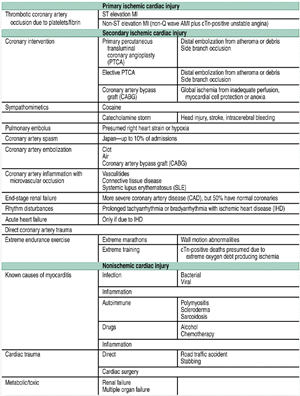 |
| Table
1. Conditions characterized by cardiac troponin elevation |
cTn
measurements are useful in three categories of patients designated in
the following discussion as STEMI, NSTEMI, and low risk.
STEMI
patients
In
patients with definite acute myocardial infarction (ST elevation MI),
a single cTn measurement taken 12 to 24 hours after admission serves to
confirm the diagnosis and indicate the degree of myocardial damage.9 The
argument is often advanced that ST segment elevation is entirely cardiac
specific and therefore biochemistry has no role to play. It has been demonstrated
in routine clinical practice, however, that the sensitivity of the ECG,
even when there is ST segment elevation, is only 95 percent.10 Clearly,
therefore, biochemical testing is needed for audit. Although studies have
demonstrated that admission cTn measurements allow further risk stratification
in patients with STEMI, there is currently no known therapeutic approach
that can be used to improve outcome in this group. Even when primary angioplasty
is used, patients presenting with STEMI who are cTn positive have a worse
outcome. For the laboratory, therefore, this means that the provision
of a 24-hour cTn service is a prerequisite for managing these patients.
Regrettably, only 10 percent of chest pain admissions receive this service.
NSTEMI
patients
The recommended management guideline for non-ST elevation patients at
high risk of ACS (non-ST elevation myocardial infarction and unstable
angina) is covered in a recent European Society of Cardiology publication.11
A pragmatic flowchart appears in Figure 1. This is based on the findings
that the response to low-molecular-weight heparins, glycoprotein IIb/IIIa
antagonists and revascularization are predicted by cTn status: only patients
who are cTn positive respond. The inability of most hospitals in the UK
to deliver a clinically appropriate service does modify the demands on
the laboratory. An ideal strategy would be to measure cTn on admission,
then 4 to 6 hours and 12 hours after admission. This would be followed
by treatment with a IIb/IIIa blocker and early intervention in cTn-positive
patients. The absence of such facilities in the UK means that a policy
based on measurement at 12 hours with subsequent treatment guided by the
cTn status at that point is probably all that is currently feasible. The
laboratory service to support the ideal approach, based on current equipment,
is possible. It does mean, however, that cTn measurement should be available
on weekends as well. If a truly treatment-targeted diagnosis were undertaken,
a 24-hour service for cTn estimation would be performed. If the strategy
were based on upstream treatment with a glycoprotein IIb/IIIa blocker
such as tirofiban prior to angioplasty,7 then a very rapid
service would be required. Ultimately this is likely to require either
a laboratory turnaround time of 30 minutes on a 24-hour basis or, more
probably, the use of point-of-care testing in selected cases.
|
|
| Figure
1. Management strategy for patients admitted with high risk for acute
cardiac syndrome (ACS). |
Low-risk
patients
Patients at low risk can be selected on clinical criteria. These are patients
without a preexisting history of coronary artery disease or atypical history
who have a normal ECG and absence of conventional risk factors. In this
group, the instance of missed myocardial infarction is typically on the
order of 5 percent,12 but a strategy based on cTn measurement
over 4 to 6 hours after admission would significantly reduce this miss
rate. At 4 hours after admission, the diagnostic sensitivity of cTn measurement
is 90 percent. Because only 5 percent of this patient group will have
an AMI, 90 percent of the group would be detected and the occurrence of
missed AMI reduced typically to less than 1 percent. Since, in the very
short term, patients with a normal ECG and a normal cTn after 4 hours
are at very low risk, this patient group can be investigated by follow-up
(next-day) cTn measurement and noninvasive testing via a rapid-access
chest pain clinic. A typical testing paradigm is illustrated in Figure
2. It is not reasonable simply to discharge these patients without some
form of follow-up, since a small percentage of this population has a cardiac
event. Providing this service is more challenging for the laboratory since
it requires, effectively, a 24-hour cTn service.
|
|
| Figure
2. Management strategy for emergency department (ED) rule-out. |
Conclusion
In conclusion, cTns have a major role in the management of patients with
chest pain, but the service configuration is dominated by the management
pathways in place. Without appropriate clinical management pathways to
triage patients according to risk group and investigate them accordingly,
the frequency and timeliness of laboratory testing is irrelevant. It is
up to the laboratory and the clinicians to define their management pathways
and the role of biochemical markers within them. It should be remembered
that the use of cTns in risk stratification is recognized by European,
British and American guidelines and also by the National Institute of
Clinical Excellence (UK). The challenge is to deliver the service.
References
1. Collinson
PO, Chandler HA, Stubbs PJ, Moseley DS, Lewis D, Simmons MD. Measurement
of serum troponin T, creatine kinase MB isoenzyme, and total creatine
kinase following arduous physical training. Ann Clin Biochem 1995;32 (Pt
5):450-3.
2. Stubbs P, Collinson
P, Moseley D, Greenwood T, Noble M. Prospective study of the role of cardiac
troponin T in patients admitted with unstable angina. [See comments.]
BMJ 1996;313:262-4.
3. Lindahl B, Venge
P, Wallentin L. Troponin T identifies patients with unstable coronary
artery disease who benefit from long-term antithrombotic protection. Fragmin
in Unstable Coronary Artery Disease (FRISC) Study Group. J Am Coll Cardiol
1997;29:43-8.
4. Hamm CW, Heeschen
C, Goldmann B, Vahanian A, Adgey J, Miguel CM, et al. Benefit of abciximab
in patients with refractory unstable angina in relation to serum troponin
T levels. c7E3 Fab Antiplatelet Therapy in Unstable Refractory Angina
(CAPTURE) Study Investigators [published erratum appears in N Engl J Med
1999 Aug 12;341(7):548]. [See comments.] N Engl J Med 1999;340:1623-9.
5. Heeschen C, Hamm
CW, Goldmann B, Deu A, Langenbrink L, White HD. Troponin concentrations
for stratification of patients with acute coronary syndromes in relation
to therapeutic efficacy of tirofiban. PRISM Study Investigators. Platelet
Receptor Inhibition in Ischemic Syndrome Management. [See comments.] Lancet
1999;354:1757-62.
6. Lindahl B, Diderholm
E, Lagerqvist B, Husted S, Kontny F, Stahle E. Invasive vs noninvasive
strategy in relation to troponin T level and ECG findings-a FRISC-2 substudy.
Eur Heart J 2000;21:469.
7. Cannon CP, Weintraub
WS, Demopoulos LA, Vicari R, Frey MJ, Lakkis N, et al. Comparison of early
invasive and conservative strategies in patients with unstable coronary
syndromes treated with the glycoprotein IIb/IIIa inhibitor tirofiban.
N Engl J Med 2001;344:1879-87.
8. Myocardial infarction
redefined-a consensus document of the Joint European Society of Cardiology/American
College of Cardiology Committee for the redefinition of myocardial infarction.
Eur Heart J 2000;21:1502-13.
9. Rao AC, Collinson
PO, Canepa-Anson R, Joseph SP. Troponin T measurement after myocardial
infarction can identify left ventricular ejection of less than 40%. Heart
1998;80:223-5.
10. Topol EJ, Bates
ER, Walton JA Jr, Baumann G, Wolfe S, Maino J, et al. Community hospital
administration of intravenous tissue plasminogen activator in acute myocardial
infarction: improved timing, thrombolytic efficacy and ventricular function.
J Am Coll Cardiol 1987;10:1173-7.
11. Bertrand ME, Simoons
ML, Fox KA, Wallentin LC, Hamm CW, McFadden E, et al. Management of acute
coronary syndromes: acute coronary syndromes without persistent ST segment
elevation. Recommendations of the task force of the European Society of
Cardiology. Eur Heart J 2000;21:1406-32.
12. Collinson PO,
Premachandram S, Hashemi K. Prospective audit of incidence of prognostically
important myocardial damage in patients discharged from emergency department.
BMJ 2000;320:1702-5.
|